Bald Patches and Hair Loss in Pets: What Could Be Behind It
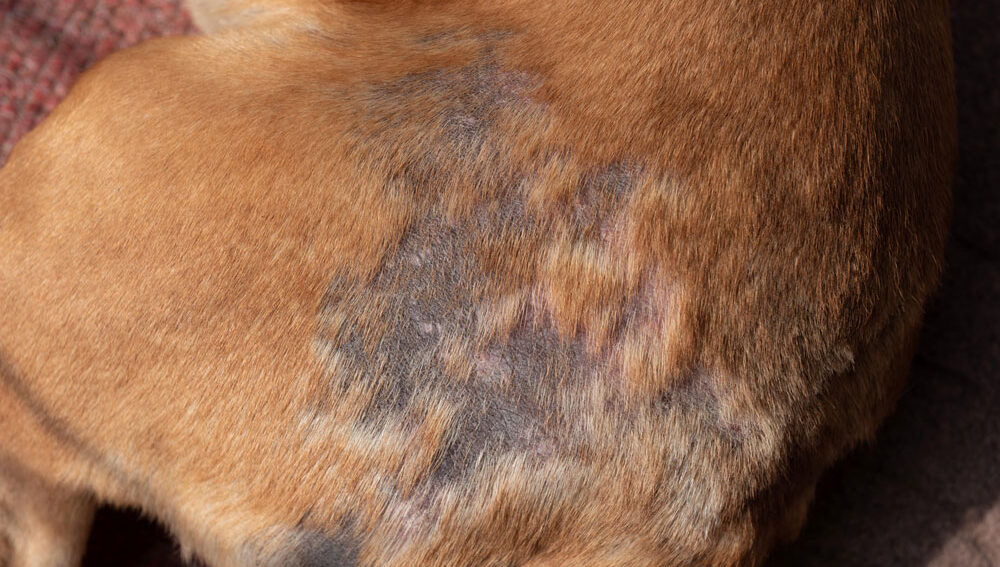
A little extra shedding is one thing. But when you start noticing actual bald patches, thinning around the flanks, bare skin on the belly, or a tail that’s looking sparse, you start to wonder. Hair loss in dogs and cats, called alopecia, is one of those symptoms that can point in a dozen different directions at once. It might be a hormone imbalance, a skin infection, an allergy, or a combination of factors. Figuring out which one requires more than guesswork.
Harbor Pines Veterinary Center in Harbor City offers the kind of thorough, AAHA-certified care that methodically works through the possibilities. Our services include dermatologic workups and comprehensive physical exams designed to find the root of the problem rather than just address the surface. Request an appointment and let’s figure out what’s going on.
What’s the Difference Between Normal Shedding and Alopecia?
Alopecia is the medical term for hair loss, and it’s a symptom rather than a disease on its own. Normal shedding is steady, distributed across the body, and follows seasonal patterns in many breeds. Alopecia is different.
Signs that hair loss warrants evaluation:
- Patchy or localized thinning outside seasonal patterns
- Bald spots with clearly defined edges
- Symmetrical thinning on both sides of the body, particularly the flanks
- Redness, scaling, or crusting on the affected skin
- Hair that doesn’t regrow within normal cycles
- Excessive scratching, licking, or chewing focused on specific areas
- Changes in hair texture alongside loss (dull, brittle, broken)
- Skin color changes (darkening, redness, or unusual pigmentation)
Hair “barbering” (where the fur is broken or damaged from licking or chewing) points in a different direction than hair falling out from the root. Knowing what the skin underneath the hair loss looks like matters as much as the hair loss itself. A bald spot with healthy-looking skin points in different diagnostic directions than a bald spot with red, inflamed, or scaly skin.
Our wellness exams include skin and coat screening as a routine part of the full physical, which is often where early changes get caught.
How Do Allergies Cause Hair Loss in Pets?
Allergies are one of the most common reasons pets develop hair loss. The mechanism is indirect: the immune system overreacts to a trigger, causing inflammation and intense itching. The scratching, licking, and chewing that follow are what damages the hair shafts and creates bald patches. The skin underneath is often red, irritated, or thickened from chronic trauma.
The major categories of allergic triggers:
- Environmental allergens including pollens, molds, dust mites, and grass. Atopic dermatitis is the umbrella term for environmental allergic skin disease in dogs.
- Food allergies to specific protein sources (beef, chicken, dairy are most common). These typically produce year-round symptoms rather than seasonal flares.
- Flea allergies, which are particularly common in mild climates. Flea allergy dermatitis is a hypersensitivity to flea saliva, where even a single bite can trigger weeks of intense itching.
Dogs and cats present allergies differently. Dogs typically itch on the face, ears, paws, belly, and armpits. Cats often show miliary dermatitis (small crusts), symmetrical hair loss on the belly and inner thighs from overgrooming, or eosinophilic granulomas.
Our allergy services include comprehensive workups for pets with recurring or chronic itch and hair loss.
Parasites and Skin Infections That Cause Hair Loss
Even indoor pets can pick up parasites, and some are too small to see without a microscope. The major parasitic causes of hair loss:
- Demodex mites: live in the hair follicles and are present in small numbers in most dogs without causing problems. Demodex overgrowth happens when the immune system isn’t keeping the population in check, producing patchy hair loss often around the face, eyes, and forelimbs.
- Sarcoptic mange (scabies): highly contagious and causes intense itching with hair loss, typically starting on the ears, elbows, and belly. It can be transmitted to humans temporarily.
- Fleas: cause hair loss directly through bite-related itch and indirectly when allergic pets develop flea allergy dermatitis. Year-round parasite prevention is key for management. Our pharmacy carries Flea & Tick prevention for dogs and Flea & Tick prevention for cats in multiple formulations.
- Ringworm: a fungal infection (not actually a worm) that creates circular bald spots, often with redness or scaling at the edges. It’s contagious to people and other pets, particularly in households with kittens.
Bacterial and yeast infections often layer on top of these primary causes. When skin becomes inflamed from any source, surface organisms can overgrow and create secondary infections.
Diagnosis of parasites and infections requires actual testing: skin scrapings for mites, cytology for bacteria and yeast, and fungal culture for ringworm. We perform these tests as part of any hair loss workup.
Hormonal Causes of Hair Loss in Pets
When hair thins symmetrically along both sides of the body without much scratching, hormones are often involved. These changes can be gradual enough to go unnoticed until they’re significant.
Thyroid and Adrenal Conditions
Hypothyroidism in dogs is one of the most common hormonal causes. Insufficient thyroid hormone affects the coat (thinning, dullness, sometimes a “rat tail” appearance), along with weight gain despite normal eating, lethargy, cold intolerance, and skin changes. Diagnosis is straightforward with a thyroid panel, and treatment with daily oral supplementation typically restores coat quality within weeks to months.
Cushing’s disease (hyperadrenocorticism) is the opposite end of the spectrum, with excessive cortisol production. The classic presentation includes symmetrical hair loss along the trunk, a pot-bellied appearance, increased thirst and urination, increased appetite, and sometimes panting. Cushing’s diagnosis requires specific endocrine testing, and treatment is medical (sometimes surgical for adrenal tumors).
Sex Hormones and Topical Medication Exposure
Intact male dogs occasionally develop symmetrical hair loss from testicular tumors producing excess estrogen. Intact females can show similar changes during heat cycles or from ovarian remnants after incomplete spays. Spaying or neutering often resolves these cases.
A less obvious cause: pets can absorb hormones from human medications applied to skin. People using hormone replacement creams, testosterone gels, or estrogen patches can transfer significant amounts to pets through skin-to-skin contact, licking application sites, or contact with treated bedding. Symmetrical hair loss in your pet, if you use topical hormones, warrants this conversation.
Why Routine Bloodwork Matters for Coat Health
Hormone imbalances often show up on blood work before they become visually obvious. Routine wellness blood panels establish a baseline that makes subtle changes easier to catch. For dogs and cats with developing coat changes, an early thyroid panel or chemistry profile often points the workup in the right direction.
Breed-Related Hair Loss Conditions
Some dogs inherit coat conditions that can’t be cured but can be managed. Knowing breed tendencies sets realistic expectations.
- Color dilution alopecia: affects dogs with dilute coat colors (blue, fawn, isabella) and produces gradual hair thinning over the diluted areas, typically starting between 6 months and 3 years of age. Common in Doberman Pinschers, Italian Greyhounds, Yorkies, and Chow Chows.
- Seasonal flank alopecia: produces symmetrical bald patches on the flanks that come and go with the seasons. Common in Boxers, English Bulldogs, and Airedales.
- Sebaceous adenitis: an immune-mediated inflammation of the oil-producing glands. Common in Standard Poodles and Akitas.
- Zinc-responsive dermatosis: affects Northern breeds (Siberian Huskies, Alaskan Malamutes) and produces crusty lesions and hair loss around the face, eyes, and pressure points.
Stress, Pain, and Overgrooming as Causes of Hair Loss
Pets, especially cats, can express emotional distress through repetitive grooming that creates smooth, thin areas. Psychogenic alopecia in cats produces symmetrical bald patches on the belly, inner thighs, and along the flanks where the cat can reach. The skin underneath usually looks completely normal, which is one of the clues that the cause is behavioral.
Common feline stressors include changes in household members, new pets, schedule disruptions, multi-cat conflict, moving, and inadequate environmental enrichment. The life stressors that affect cats often look minor from a human perspective but matter enormously to the cat.
Dogs show similar patterns through repetitive licking of one spot, often a paw or wrist. Over time, this creates a lick granuloma, a thickened, hairless, and sometimes ulcerated area that’s notoriously hard to break.
Pain is another commonly overlooked driver of overgrooming. Pets lick, chew, or pull hair over areas that hurt even when the skin looks fine. Common pain-related grooming patterns:
- Lower belly licking in cats with feline idiopathic cystitis or other urinary issues
- Hip or back licking in dogs and cats with osteoarthritis
- Localized licking over specific painful joints or muscles
Pain-driven and stress-driven grooming can look identical, which is why diagnostics matter. Treating the underlying cause (anxiety management, pain control, environmental changes, treating cystitis) usually resolves the grooming behavior, and the hair regrows.
How Does Nutrition Affect Your Pet’s Coat Health?
The skin and coat are among the first places nutritional shortfalls show up. Hair growth requires a steady supply of protein, fatty acids, zinc, and biotin. Diets that skimp on any of these (or pets who don’t absorb them well due to GI issues) often show coat changes before other signs.
A complete and balanced diet appropriate for the pet’s life stage is the foundation. For pets with diagnosed skin conditions or breed-related coat issues, prescription skin and coat care diets provide therapeutic levels of supportive nutrients beyond what standard maintenance diets offer. Omega fatty acid supplementation can help restore skin and coat health and reduce allergy symptoms when given regularly long-term.
What Happens During a Hair Loss Workup?
Reducing anxiety about a vet visit starts with knowing what to expect. A typical alopecia workup includes:
- Detailed history: timing of onset, distribution of hair loss, level of itching, recent diet or environment changes, and other symptoms
- Physical exam and pattern mapping: documenting where hair loss is, what the skin underneath looks like, and any concurrent findings
- In-house testing: skin scrapings for mites, cytology for bacterial and yeast organisms, hair pluck examination, Wood’s lamp evaluation for ringworm
- Fungal culture when ringworm is suspected (results take 1 to 4 weeks)
- Bloodwork and endocrine panels when hormonal causes are suspected
- Allergy evaluation through elimination diets for food allergies or formal allergy testing for environmental allergens
- Biopsy for cases where diagnosis remains unclear after the initial workup
Our in-house lab capabilities provide rapid results for cytology, scrapings, and basic bloodwork, so treatment decisions don’t wait on outside lab turnaround.

How Hair Loss Is Treated
Because so many different conditions cause alopecia, treatment is always matched to the specific diagnosis:
- Allergies: combination of medicated baths, omega-3 supplementation, prescription anti-itch medications, environmental management, and sometimes immunotherapy
- Parasites: targeted antiparasitic treatments and ongoing year-round prevention
- Bacterial or yeast infections: topical and/or systemic antimicrobials based on cytology results
- Hormonal conditions: specific hormone replacement (thyroid) or modulation (Cushing’s, hyperthyroidism)
- Stress-related grooming: anxiety management, environmental enrichment, sometimes medication, and treating any underlying medical cause
- Pain-related grooming: pain management for the underlying source
- Nutritional gaps: diet adjustment with veterinary nutrition input
Follow-up rechecks confirm regrowth, fine-tune medications, and catch secondary issues before they become significant. Most cases need at least one follow-up visit, and chronic conditions need ongoing monitoring.
For pets or families who can’t easily come into the clinic, our mobile services bring care directly to their home.
Frequently Asked Questions About Pet Hair Loss
Is hair loss always a sign of something serious?
Not always, but it’s always worth investigating. Some causes are minor and easily managed; others are early signs of significant systemic disease. A workup gives you a definitive answer rather than continued guessing.
Will my pet’s hair grow back?
In most cases, yes, once the underlying cause is identified and treated. Some breed-related conditions involve permanent or recurrent loss in specific areas. Hormone-related and infection-related hair loss typically regrows fully with appropriate treatment.
Can I treat hair loss with over-the-counter pet store products?
Sometimes for very mild surface issues, but not for cases that have persisted, are spreading, or include skin changes underneath. The wrong product on the wrong condition often makes things worse.
How long does treatment usually take?
Variable by cause. Bacterial infections often clear in 3 to 4 weeks. Ringworm requires 6 to 12 weeks. Hormonal conditions need ongoing management. Most pets show meaningful improvement within the first few weeks even when full resolution takes longer.
Restoring Your Pet’s Coat Health
Most cases of hair loss improve significantly once the cause is identified and treated. Whether your pet is scratching openly, quietly overgrooming, or showing symmetrical thinning that came on gradually, there’s a clear path forward. The pets who do best are the ones whose families stop guessing and bring them in for a methodical workup.
Our team at Harbor Pines provides thorough diagnostic evaluation and personalized treatment plans for every pet we see. If you’ve noticed coat changes that aren’t normal for your pet, schedule a visit. We’ll work through the possibilities together until we have a real answer and a real plan.