
A tick is an unpleasant and unwelcome sight, especially when the parasite is attached to your beloved pet. To minimize disease transmission and stop the tick life cycle, prompt removal is necessary. Unfortunately, these small and unsavory creatures can be difficult to extract, which can be frustrating and stressful for your pet and you. To learn how to remove a tick safely from your pet, read our Harbor Pines Veterinary Center team’s tips and get the answers to your frequently asked tick removal questions.
Question: Why are ticks hazardous to pets?
Answer: Ticks are vectors (i.e., carriers) for many harmful bacteria species, including those that cause Lyme disease, anaplasmosis, ehrlichiosis, Rocky Mountain spotted fever, and many more. Ticks initially ingest the infectious material while feeding on wildlife (e.g., mice, deer, squirrels). During their next blood meal, these parasites then transmit diseases to pets and humans through their saliva.
Although tick-borne diseases are generally treatable, their vague presentation can delay diagnosis, chronically affecting pets who then suffer permanent injury. Depending on the disease, health consequences vary but may include joint stiffness, fever, lethargy, lymph node enlargement, bleeding disorders, kidney damage, and neurologic dysfunction.
Q: Will tick removal hurt my pet?
A: Proper removal may cause your pet mild and brief discomfort as an attached tick’s mouthparts are pulled from your four-legged friend’s skin. Pain typically only occurs because of improper removal if a pet’s skin or hair is pulled or pinched. Using a specially designed tick removal tool is the best way to ensure a secure and safe grip, and pain-free removal.
Q: Is it safe to burn or twist the tick off my pet?
A: No. These methods are outdated and can cause your pet additional pain or injury. They are not recommended under any circumstances. Manual removal with tweezers or a tick removal tool is the only way to remove a tick safely and humanely from your pet.
Q: How do I remove a tick from my pet?
A: After finding a tick attached to your pet, take your four-legged friend to a quiet distraction-free location. Place small pets on a table or furniture to ensure easy access and safe restraint. Part your pet’s hair so you have a clear work area, and using your removal tool, slide under the tick and grasp its head close to the skin’s surface. If you’re using tweezers or a hemostat, ensure you do not pinch your pet’s skin and hair. Pull up and away using steady gentle pressure. You may feel a small pop as the tick is freed. Check your pet’s skin to ensure you have removed the tick’s head and mouthparts.
Q: The tick’s head is stuck in my pet’s skin. What should I do?
A: If the tick’s body is broken during removal, its head or mouthparts may be embedded in your pet’s skin. If your pet will tolerate additional handling and if the remaining parts are large enough for you to grasp with your removal tool, you may be able to remove the parasite’s fragments. If this isn’t possible, monitor the area for several days while the trapped pieces dry up and fall out. If your pet’s skin is visibly irritated, itchy, or swollen after several days or if the tick’s head remains embedded, contact our Harbor Pines Veterinary Center team.
Q: How can I safely dispose of the tick I removed from my pet’s skin?
A: Properly disposing of live ticks is crucial to prevent them from reattaching or reproducing in the environment. The best options minimize handling, so you avoid contact with potentially infectious material. To dispose of a live tick properly, follow one of these tips:
- Flush the tick in the toilet
- Wrap the tick in tape
- Seal the tick in a plastic bag
- Drown the tick in isopropyl alcohol
Dead or desiccated ticks can be disposed of safely in a trash can. Wash your hands thoroughly after handling a tick, tick tools, and your pet.
Q: Should I have my pet tested for tick-borne diseases?
A: Tick-borne disease testing is available for dogs and recommended as part of their annual wellness testing. The test detects tick-borne disease antibodies (i.e., proteins) in a dog’s blood, indicating exposure, but not necessarily that they have contracted a disease. If your pet tests positive and is exhibiting signs, your veterinarian will recommend antibiotic treatment. Tick-borne disease testing is not necessary after a single tick bite unless your pet exhibits concerning signs several weeks or months after exposure.
Q: How can I identify the tick that bit my pet?
A: Although identifying a tick’s species isn’t necessary, you may be curious about your region’s tick populations and your pet’s potential disease risks. To identify a tick you removed from your pet’s skin, visit TickSpotters, upload a picture, and answer a few questions about your pet’s encounter.
Q: My pet receives tick prevention: Why am I finding live ticks on my pet? 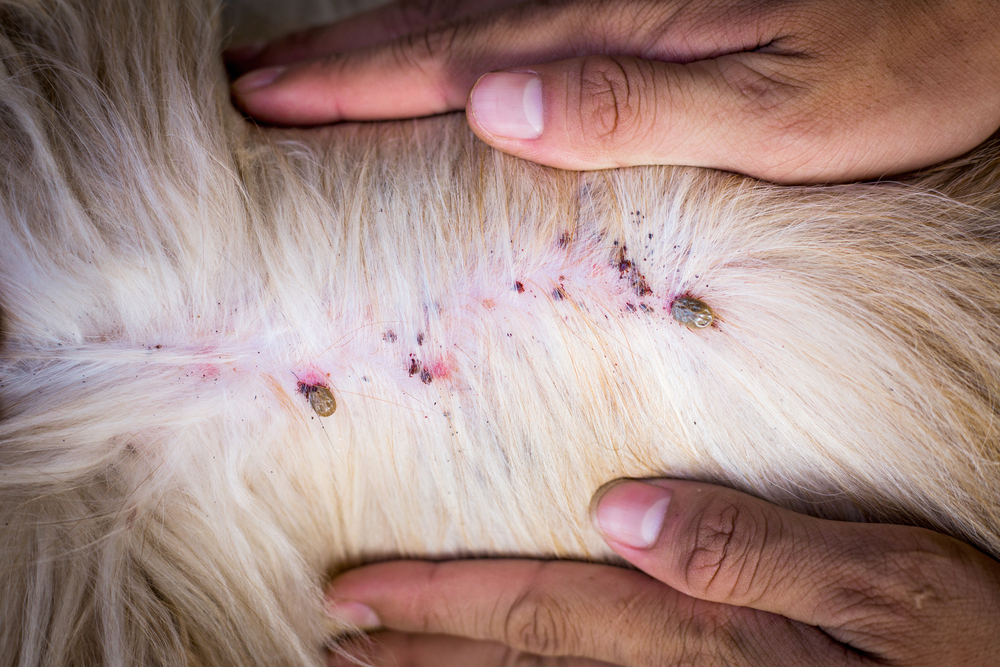
A: Most tick preventive products kill a tick after it bites your pet, rather than completely repelling the parasites. As such, you will occasionally see a tick attached to your pet. These ticks are generally newly attached or dying. Veterinary-recommended tick preventives are designed to kill ticks before disease transmission, usually fewer than eight hours after attachment.
An engorged (i.e., swollen) tick attached to your pet has ingested a blood meal, indicating a problem with your four-legged friend’s prevention plan. This is generally attributable to forgotten or late dosing, or inappropriate application, rather than the product being completely ineffective. If you’re concerned about your pet’s tick preventive efficacy, contact your Harbor Pines Veterinary Center veterinarian.
Although tick-borne diseases are generally treatable, their vague presentation can delay diagnosis, chronically affecting pets who then suffer permanent injury. To prevent your pet from becoming an easy target for disease-carrying ticks, contact our Harbor Pines Veterinary Center team to ensure your pet is receiving effective parasite prevention.
